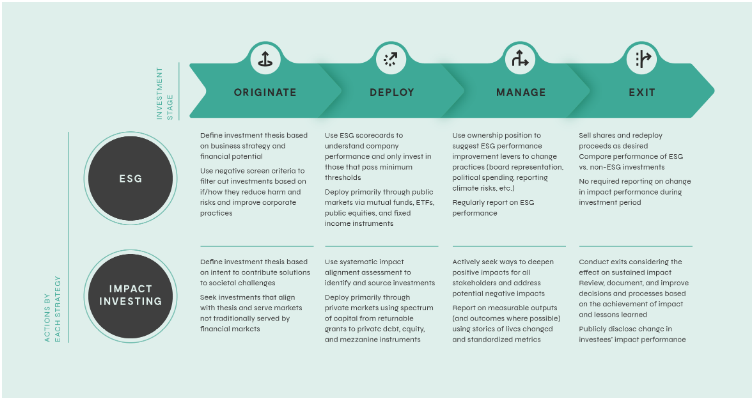
Disparities in Medicare Advantage vs. Traditional Medicare Care – BIOENGINEER.ORG

Report on Racial and Ethnic Disparities in Medicare and Alignment with Sustainable Development Goals
Introduction: Healthcare Inequity as a Barrier to Sustainable Development
A recent study led by Tipirneni, R. investigates significant racial and ethnic disparities in preventive and chronic disease care between Medicare Advantage and Traditional Medicare plans. These findings present a critical challenge to the achievement of key United Nations Sustainable Development Goals (SDGs), particularly SDG 3 (Good Health and Well-being) and SDG 10 (Reduced Inequalities). This report analyzes the study’s findings through the lens of these global goals, highlighting systemic failures and outlining necessary actions to foster health equity.
Analysis of Findings in the Context of SDGs
Challenges to SDG 3: Good Health and Well-being
The research reveals that disparities in healthcare access and outcomes directly undermine the core principle of SDG 3, which aims to ensure healthy lives and promote well-being for all at all ages. The study identifies specific failures in the U.S. Medicare system that disproportionately affect minority populations.
- Ineffective Chronic Disease Management: Medicare Advantage plans, despite their design, often fail to provide adequate preventive services for chronic conditions such as diabetes, hypertension, and cardiovascular diseases. This gap in care for vulnerable populations is a direct impediment to achieving universal health coverage (Target 3.8).
- Barriers to Preventive Care: Beneficiaries in Medicare Advantage plans were found to experience more significant barriers to receiving timely and appropriate preventive care compared to those in Traditional Medicare. This disparity limits progress toward reducing premature mortality from non-communicable diseases (Target 3.4).
- Lack of Patient Engagement: The research indicates that lower levels of patient engagement and shared decision-making among minority groups lead to poorer health outcomes. Empowering patients is essential for a people-centered approach to health, a cornerstone of SDG 3.
Implications for SDG 10: Reduced Inequalities
The study’s findings are a stark illustration of the inequalities that SDG 10 seeks to eliminate. The disparities are not random but are rooted in systemic and social factors that perpetuate unequal outcomes based on race and ethnicity.
- Systemic Disparities: The research demonstrates how different healthcare financing models (Medicare Advantage vs. Traditional) can exacerbate existing inequalities, failing to ensure equal opportunity and reduce inequalities of outcome (Target 10.3).
- Socioeconomic Determinants of Health: The report underscores that health outcomes are deeply intertwined with socioeconomic factors, including financial constraints, transportation, and health literacy. Addressing these social determinants is crucial for promoting the social inclusion of all, irrespective of origin or economic status (Target 10.2).
- The Digital Divide: While telehealth offers potential benefits, its integration into Medicare plans raises concerns about the digital divide. Unequal access to technology threatens to create new layers of inequality, further marginalizing vulnerable communities and working against the goals of SDG 10.
- Cultural Competence Gaps: A lack of cultural competence among healthcare providers was identified as a significant contributor to health disparities. This highlights the need for institutional practices that are sensitive and responsive to the diverse needs of all populations.
Recommendations for Achieving Health Equity and Advancing the SDGs
A Multi-faceted Strategy for Institutional Reform (SDG 16 & SDG 17)
To address the disparities identified and align healthcare practices with the SDGs, a comprehensive approach is required. This involves building effective, accountable, and inclusive institutions (SDG 16) and fostering multi-stakeholder partnerships (SDG 17).
Key Areas for Intervention
- Policy Reform: Policymakers must reassess Medicare frameworks to ensure they actively mitigate, rather than perpetuate, health inequalities. This includes targeted interventions aimed at improving care delivery within Medicare Advantage plans.
- Community-Based Interventions: Collaboration between healthcare providers, insurers, and community organizations is vital to address the social determinants of health and build trust with marginalized communities.
- Education and Training: Mandatory cultural competence training for healthcare personnel must be implemented to improve patient-provider communication and health outcomes.
- Data and Technology Integration: Leverage data analytics to identify and address disparities in real-time. Technology must be deployed equitably to close, not widen, the access-to-care gap.
Conclusion: A Call to Action
The research by Tipirneni et al. serves as a critical call to action. The persistence of racial and ethnic disparities within the Medicare system is a significant barrier to achieving a just and sustainable future as envisioned by the SDGs. Addressing these inequities is not merely a healthcare issue but a fundamental requirement for upholding human rights and fulfilling the global commitment to leave no one behind. Stakeholders at all levels must act decisively on these findings to build a healthcare system that promotes health and well-being for all.
Analysis of Sustainable Development Goals in the Article
1. Which SDGs are addressed or connected to the issues highlighted in the article?
-
SDG 3: Good Health and Well-being
The article’s central theme is healthcare, focusing on preventive care, chronic disease management (diabetes, hypertension, cardiovascular diseases), and achieving equitable health outcomes. It directly addresses the goal of ensuring healthy lives and promoting well-being for all by highlighting disparities that prevent this for certain racial and ethnic groups.
-
SDG 10: Reduced Inequalities
The entire study is framed around “racial and ethnic disparities” and “health inequalities.” It scrutinizes how systemic factors within the Medicare system contribute to unequal health outcomes, directly aligning with the goal of reducing inequality within and among countries. The call to mitigate these disparities is a core message.
-
SDG 16: Peace, Justice and Strong Institutions
The article critiques the effectiveness of current healthcare frameworks (Medicare Advantage vs. Traditional Medicare), which are institutional structures. It calls for policymakers to reassess these frameworks and for healthcare systems to foster a “culture of accountability and responsiveness,” which relates to the development of effective, accountable, and transparent institutions.
-
SDG 17: Partnerships for the Goals
The conclusion of the analysis within the article explicitly calls for a “multi-faceted approach that includes policy changes, educational initiatives, and community-based interventions.” It emphasizes that “collaboration among healthcare providers, insurers, and community organizations will be vital,” which directly reflects the spirit of creating partnerships to achieve sustainable development goals.
2. What specific targets under those SDGs can be identified based on the article’s content?
-
SDG 3: Good Health and Well-being
- Target 3.4: By 2030, reduce by one-third premature mortality from non-communicable diseases through prevention and treatment. The article’s focus on disparities in managing chronic diseases like “diabetes, hypertension, and cardiovascular diseases” and its emphasis on the failure to provide “necessary preventive services” directly relates to this target.
- Target 3.8: Achieve universal health coverage, including financial risk protection, access to quality essential health-care services…for all. The article examines barriers that limit the ability of minority groups to receive “timely and appropriate care” under different Medicare plans, questioning the real-world effectiveness of these plans in providing equitable access to healthcare for all.
-
SDG 10: Reduced Inequalities
- Target 10.2: By 2030, empower and promote the social, economic and political inclusion of all, irrespective of…race, ethnicity…or other status. The research highlights how racial and ethnic minorities are disproportionately affected by gaps in care, and calls for an equitable system that serves all individuals, promoting their inclusion in receiving quality healthcare.
- Target 10.3: Ensure equal opportunity and reduce inequalities of outcome… The study’s main purpose is to identify “unequal health outcomes” resulting from the current Medicare framework. It calls for policy changes and interventions aimed at “reducing health disparities” to ensure more equal outcomes.
-
SDG 16: Peace, Justice and Strong Institutions
- Target 16.6: Develop effective, accountable and transparent institutions at all levels. The article questions the effectiveness of Medicare Advantage plans and calls for a “reassessment of current frameworks.” The mention of using data analytics to foster a “culture of accountability and responsiveness within healthcare systems” aligns with strengthening institutional performance.
-
SDG 17: Partnerships for the Goals
- Target 17.17: Encourage and promote effective public, public-private and civil society partnerships. The article explicitly states that tackling the identified disparities requires “collaboration among healthcare providers, insurers, and community organizations,” which is the essence of this target.
3. Are there any indicators mentioned or implied in the article that can be used to measure progress towards the identified targets?
-
For Target 3.4 (Reduce mortality from non-communicable diseases):
The article implies indicators by focusing on specific diseases. Progress could be measured by tracking the prevalence, management, and mortality rates associated with “diabetes, hypertension, and cardiovascular diseases,” specifically disaggregated by racial and ethnic groups within the different Medicare plans.
-
For Target 3.8 (Achieve universal health coverage):
The article points to several indicators. These include rates of access to and utilization of “preventive care” and “timely and appropriate care” among different demographic groups. Another implied indicator is the “digital divide” in telehealth, which can be measured by tracking telehealth service usage across populations with varying levels of technology and internet access.
-
For Target 10.3 (Reduce inequalities of outcome):
The primary indicator is the disparity in health outcomes itself. The article suggests measuring “gaps in care that disproportionately affect minority groups” and comparing “health outcomes across various demographics.” This would involve statistical analysis of health indicators between different racial and ethnic groups to measure the reduction of these gaps over time.
-
For Target 16.6 (Develop effective institutions):
An implied indicator for institutional effectiveness would be the reduction in the health disparities identified in the study following policy changes. Measuring the change in health outcomes for minority groups after interventions are implemented would serve as a measure of the healthcare system’s accountability and responsiveness.
4. Summary Table of SDGs, Targets, and Indicators
| SDGs | Targets | Indicators |
|---|---|---|
| SDG 3: Good Health and Well-being |
3.4: Reduce premature mortality from non-communicable diseases through prevention and treatment.
3.8: Achieve universal health coverage and access to quality essential healthcare services for all. |
– Prevalence and mortality rates from diabetes, hypertension, and cardiovascular diseases, disaggregated by race and ethnicity.
– Rates of utilization of preventive care services among different demographic groups. |
| SDG 10: Reduced Inequalities |
10.2: Empower and promote the social inclusion of all, irrespective of race or ethnicity.
10.3: Ensure equal opportunity and reduce inequalities of outcome. |
– Comparative statistics on health outcomes (e.g., disease control, life expectancy) between different racial and ethnic groups.
– Measurement of “gaps in care” that disproportionately affect minority groups. |
| SDG 16: Peace, Justice and Strong Institutions | 16.6: Develop effective, accountable and transparent institutions at all levels. | – Measured reduction in health disparities following the implementation of policy changes and interventions within the healthcare system. |
| SDG 17: Partnerships for the Goals | 17.17: Encourage and promote effective public, public-private and civil society partnerships. | – Number and effectiveness of collaborations formed among healthcare providers, insurers, and community organizations to address health disparities. |
Source: bioengineer.org

What is Your Reaction?
 Like
0
Like
0
 Dislike
0
Dislike
0
 Love
0
Love
0
 Funny
0
Funny
0
 Angry
0
Angry
0
 Sad
0
Sad
0
 Wow
0
Wow
0















































:focal(1500,1000)/https://media.globalcitizen.org/a6/9a/a69a4720-d8a1-4715-b596-18738d03c05c/rotary_polio_hero_image.jpg?#)






/countries/sri-lanka/photo-credit---dmc-sri-lanka.tmb-1200v.jpg?sfvrsn=dc298bcc_1#)